In a recent wide ranging hearing, Texas legislators heard from experts and advocates on the current challenges and possible solutions to improve the health of pregnant women and babies in Texas. We appreciate the House Public Health committee identifying the health of infants as a key indicator for the overall health of a community and seeking out effective policy solutions.
Our own Adriana Kohler urged the legislature to consider expanding and streamlining access to Medicaid for pregnant women to close the gap between the time a woman discovers she’s pregnant and she enters into prenatal care. You can read more about this and other key points in her testimony and her recent op-ed titled "For Healthy Babies, Moms Need More than Google Searches.”
The Texas Observer highlighted in their coverage of the hearing the need to work on racial disparities in birth outcomes, highlighting that African American babies are twice as likely to die in their first year of life compared to other babies in Texas.
The Houston Chronicle summarized testimony from the hearing focusing on legislators’ interest in expanding access to LARCs (Long Acting Reversible Contraceptives), such as IUDs and implants, to reduce unplanned pregnancies and allow women to plan pregnancies after they have addressed other health needs that can put their pregnancy at risk.
While it didn’t receive much media attention, we were very pleased to hear state officials announce at the hearing that the new Healthy Texas Women program will cover screening and treatment for postpartum depression. Since postpartum depression impacts about 1 in 7 Texas women every year, access to early screening and treatment is key to improving mom’s health and a baby’s health and development. Postpartum depression can impact the development of a secure attachment between mother and child.
The full presentation by HHSC and DSHS is available here.
The hearing -- which is summarized below along with a few slides from the HHSC/DSHS presentation -- provided a launching pad for working on this critical issue as we head towards the next legislative session. We look forward to continuing to work with legislators, HHSC, DSHS, and others to ensure that women have the support they need to have healthy pregnancies and babies.
Texas Legislature House of Representatives
Public Health Committee Birth Outcomes Hearing
May 19, 2016
Chair: Rep. Myra Crownover
I. Invited Testimony provided by five speakers
- Lesley French, Associate Commissioner of Women’s Health Services and Evelyn Delgado Assistance Commissioner on behalf of Texas Department of State Health Services (TX DSHS)
- Dr. Lisa Hollier, Director of the Texas Children’s Hospital Center for Women and Children
- Dr. David Lakey, Associate Vice Chancellor for Population Health at The University of Texas System - The University of Texas System,
- Dr. Charleta Guillory, Texas Children’s Hospital and the March of Dimes.
Commissioners French and Delgado highlighted:
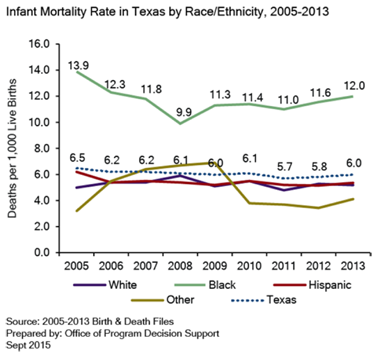
- Current birth outcomes data, which are available from the Texas State Data Center, including decreases in teen births and slight decreases in infant mortality and disparities in infant mortality, preterm birth and low birth weight babies between ethnicities and regions.
The slide above, presented by DSHS during the hearing, shows the infant mortality rate by racial and ethnic group in Texas. African American infants die at twice the rate of the state average. The legacy of systematic racism, high uninsured rates, late entry into prenatal care, and poor pre-pregnancy health have been suggested as potential causes of this large disparity.
- Late entry into prenatal, unplanned pregnancy, and preconception health as targets for action.
The DSHS slide above shows the ethnic breakdown of women who received late or no prenatal care. Both Hispanic and African American women are more likely to be uninsured and enter prenatal care later than White women. Streamlining eligibility and enrollment processes that allow for easy entry into publicly funded programs may help close this gap.
- Programs offered by DSHS including Someday Starts Now (preconception health), Healthy Texas Women (family planning and basic reproductive health services), and efforts to increase access to long acting reversible contraceptives (LARCs).
- Efforts to streamline enrollment between programs to improve usage during the period between pregnancies.
- The Healthy Texas Women program, which launches in July 2016, will cover screening and treatment for postpartum depression, including medication and counseling in the primary care setting.
Dr. Hollier offered testimony on the unique medical home model offered at the Center for Women and Children in Houston. Her testimony included:
- Underlying principles of a patient-centered, coordinated medical home model.
- Therapies offered to women to reduce prematurity including the usage of 17P, Centering Pregnancy for prenatal care, referrals to the Nurse Family Partnership, and mental health screenings.
- Patients report being very satisfied with the model.
- Policy recommendations to support for the development of medical home models to support prenatal and preconception care, expanded access to preventive health screening, improved screening for perinatal depression, efforts to increase early prenatal care usage and support for broader LARC usage.
Dr. David Lakey, former DSHS Commissioner and current UT System Vice-Chancellor, highlighted the importance of looking at systemic barriers to improving birth outcomes. He noted:
- Late or no prenatal care is an issue with both systemic and individual causes.
- Planned pregnancies can improve prenatal care access.
- Health concerns – including tobacco and substance use and mental health – must be addressed prior to pregnancy.
- Texas has participated in collaboratives with other states to identify best practices including the COIN group.
- Texas Collaborative for Healthy Mothers and Babies has focused on improving perinatal outcomes through a quality improvement initiative to reduce failed inductions and early elective deliveries.
Dr. Charleta Guillory spoke on behalf of the March of Dimes, focusing on the long-term impacts of preterm and low birthweight births. She emphasized:
- Community-based interventions that work through faith-based organizations and lay health advisors.
- The impact of low birthweight babies and preterm birth on families.
- The need for a national and state-level focus on addressing preventable poor birth outcomes.
II. Public Testimony Provided by 4 Groups
In addition to testimony by Adriana Kohler, public testimony was offered by Dr. Carl Dunn on behalf of the Texas Women’s Healthcare Coalition. Dr. Dunn discussed the importance of planning pregnancies and access to family planning before and between pregnancies. Dr. Dunn also shared that LARCs can be difficult for small practices to use because currently they are provided through the Texas Women’s Health program as a pharmacy benefit requiring patients to come back for a second appointment after the LARC has been ordered from the state.
The Texas Council on Domestic Violence shared information on the impact of intimate partner violence on birth outcomes and delayed access to prenatal care.
Olga Rodriguez from the Texas Association of Community Health Centers testified about the impact of improved prenatal care on birth outcomes in the populations served by federally qualified health centers. She noted that Certified Application Counselors (CACs) at health centers help clients apply for Marketplace or Medicaid coverage. Regarding the process to apply for and enroll in Medicaid coverage, health centers have seen situations where a pregnant woman may not be able to get prenatal care until she is five months along.
III. Legislator Comments and Questions
- The legislators, notably Rep. Sarah Davis and Chair Crownover, were very focused on improving LARC usage among women receiving publicly funded family planning care.
- Rep. Davis was also very interested in reducing tobacco and opioid usage during pregnancy, and asked several of the speakers about their experience with patients who were abusing substances.
- Rep. Elliot Naishtat asked questions concerning the availability of providers in the Texas Women’s Health program and the potential impact of domestic violence on pregnancy outcomes. He also asked about specific ways to streamline the Medicaid application and enrollment process so women receive prenatal care earlier.